
Lightbeam Health helps health plans, ACOs, and provider organizations turn fragmented clinical, claims, and quality data into coordinated action. Our Value-Based Care Operating System strengthens payer-provider alignment, improves risk adjustment accuracy, and reduces total cost of care with clear visibility into revenue performance.
Venetian Convention
& Expo Center
Dashboards don’t change performance. Action does.
Lightbeam AI moves beyond predictive analytics to deliver prescriptive, explainable recommendations that help organizations improve Stars, RAF accuracy, and total cost of care with clear line of sight to financial results.
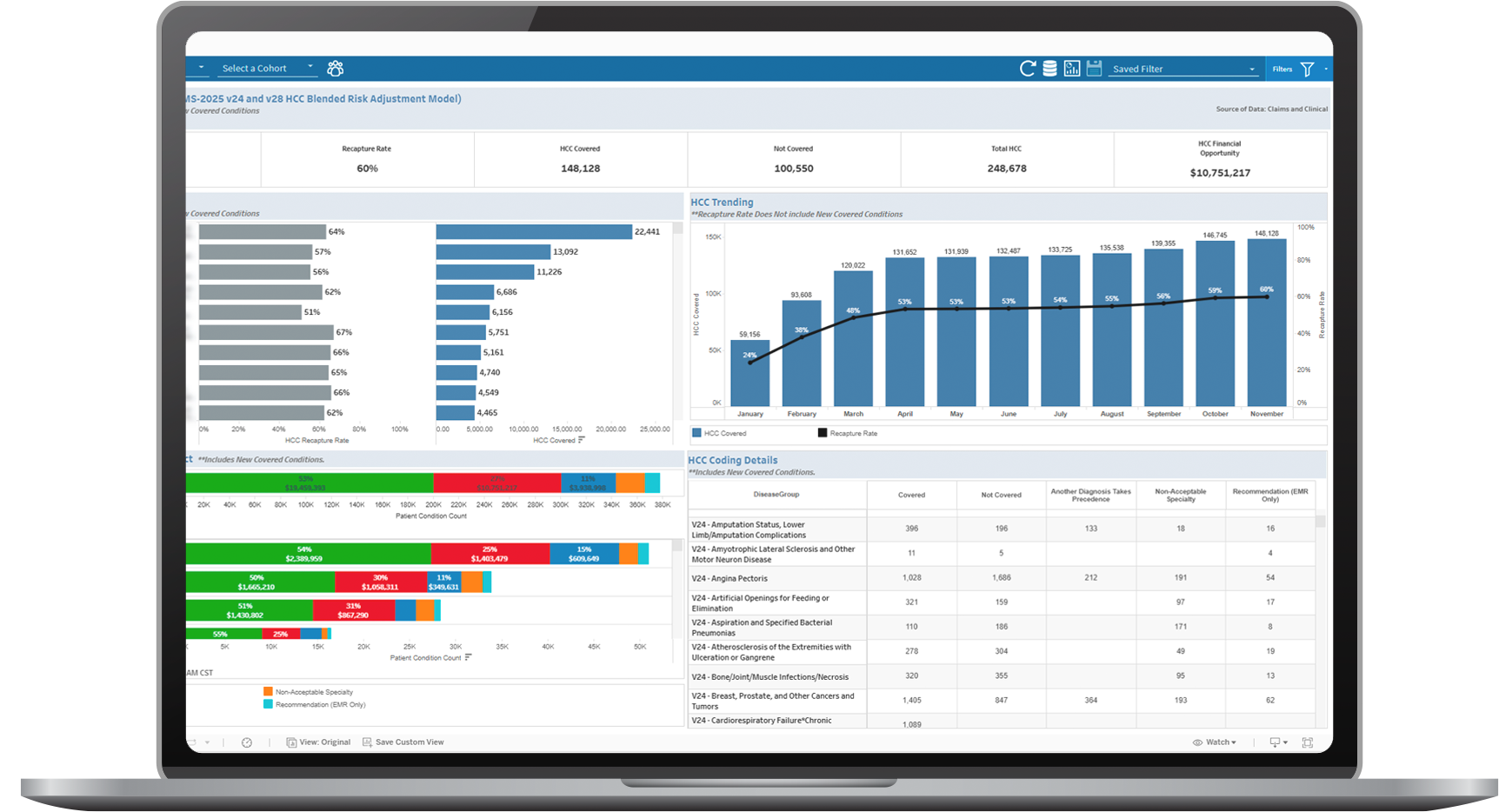
- CMS V28-aware risk adjustment analytics designed for evolving Medicare Advantage requirements
- Rising-risk patient identification to enable earlier, targeted intervention
- Integrated digital quality measures (dQMs) and ECDS reporting to streamline CMS quality programs
- Unified payer-provider performance dashboards that create a shared quality and financial signal
- Total cost of care analytics tied directly to contract performance
- Integrated deviceless remote patient monitoring (RPM) to engage high-risk members and close care gaps between visits
This isn’t just another analytics layer. It’s an operational engine that connects clinical insight to measurable financial performance.
Healthcare leaders are navigating increasing CMS scrutiny, equity requirements, and margin pressure. Lightbeam AI ties quality and risk performance directly to revenue impact, giving executive teams confidence that improvement efforts translate into durable financial results.
Lightbeam AI serves as:
- A proactive margin defense strategy for Medicare Advantage and MSSP
- A scalable population health management platform
- A contract performance engine for payer-provider collaboration
- A foundation for enterprise value-based care transformation
Moves beyond predictive analytics to recommend next-best actions for patients with modifiable behaviors.
Engage patients at scale via SMS, IVR, or AI agents, without apps or devices.
Population health strategists and RN advisors ensure you hit contract targets and maximize ROI.
Surfaces care gaps, coding opportunities, and automates reporting inside the EMR workflow.
Scale patient panels from 1:50 to 1:500+ without adding FTEs.
Uses transparent, shared assumptions so payer and provider teams can evaluate risk arrangements, negotiate faster, and track earnings vs. downside exposure off the same financial view.
A large Integrated Delivery Network (IDN) in the Southwest reduced avoidable admission events by 5.3%, and the risk of avoidable admissions by 43% among its Medicaid members by using Lightbeam AI’s 30-day Avoidable Admission model.
Learn how a rural MSSP ACO with limited resources and small teams spread across the region reduced avoidable admissions amongst a challenging population. Discover how the ACO integrated AI and a care management module into its workflow.
Discover how Midwest Health System transformed their care management strategy with Deviceless Remote Patient Monitoring, centralized 24/7 care management teams, and streamlined workflows to reach more patients, faster, and with less resources.
Visit our team at Booth #4053 to discuss your value-based care strategy, Medicare Advantage performance goals, and risk-based contract optimization. Whether you represent a payer, provider organization, or integrated delivery network, we’ll tailor the conversation to your population health and financial priorities.
Experience the Value-Based Care Operating System at Booth #4053
"*" indicates required fields