Break Free of Capacity
Constraints with
Care Orchestration
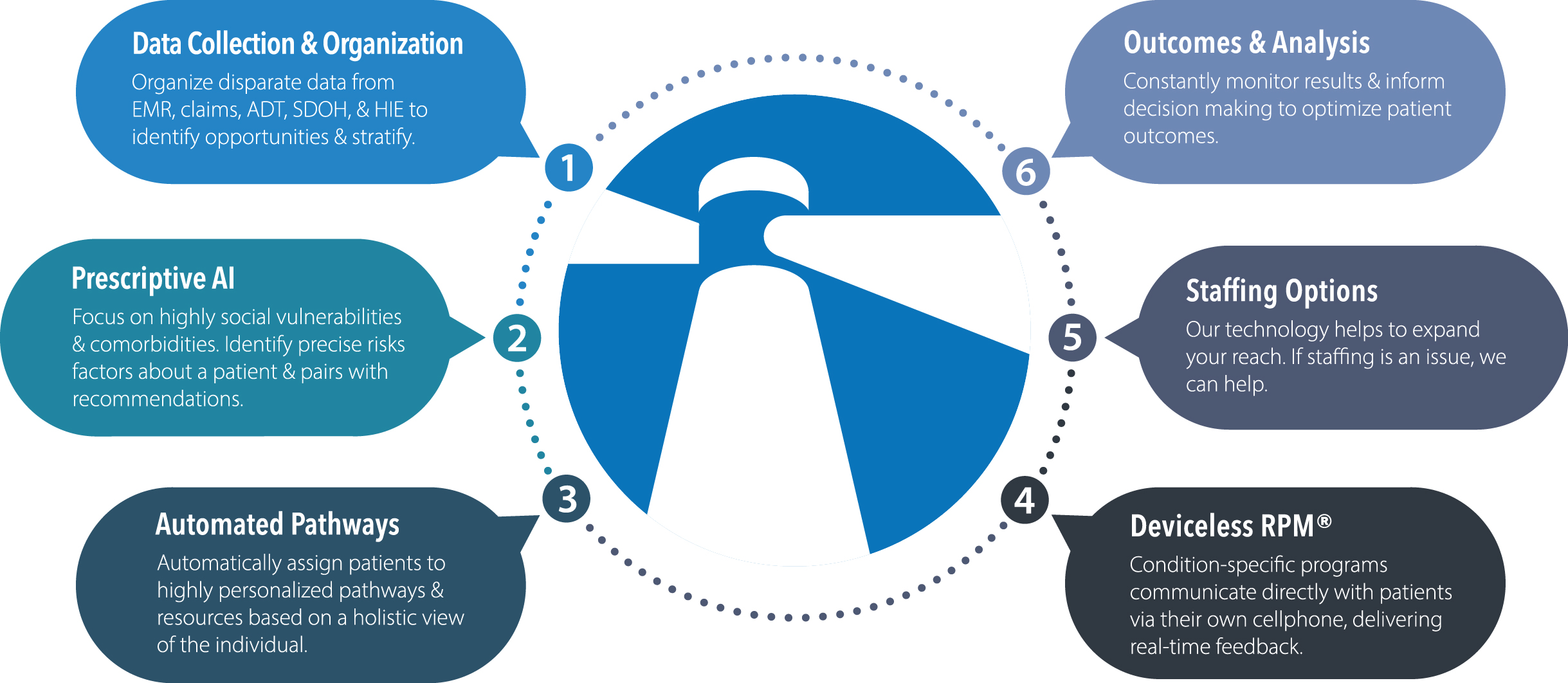
Lightbeam provides the efficiency necessary to achieve superior outcomes while mitigating burnout.
Where traditional population health management solutions stop, Lightbeam excels, providing organizations with the means to act and drive greater outcomes at scale.