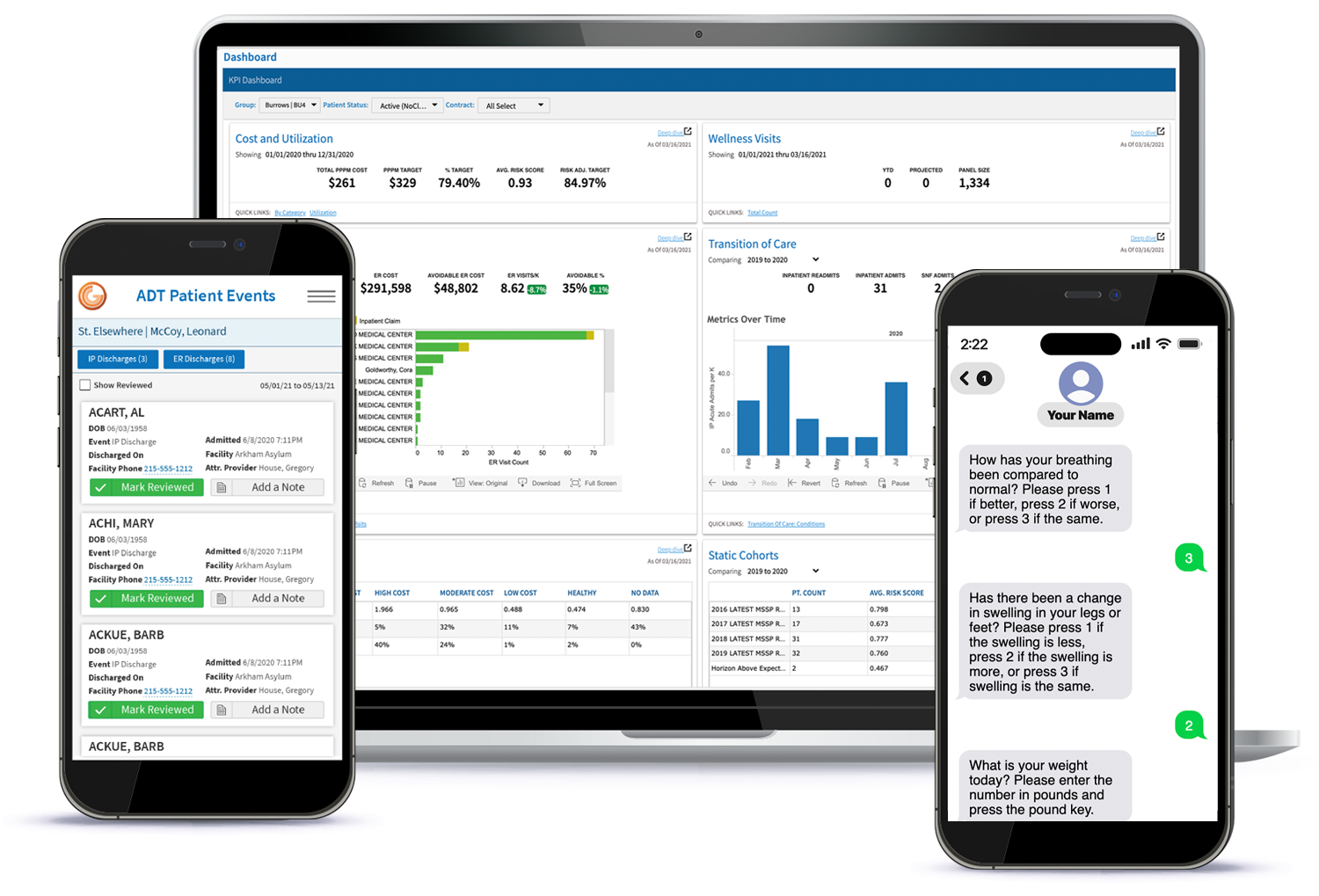
Actuarial Intelligence for Value-Based Contracts
Syntax turns value-based performance into financial truth so payers and providers can design, negotiate, and manage contracts with confidence.

Most organizations run value‑based care with fee‑for‑service tools like spreadsheets and payer reports, which creates blind spots in contract economics, unmodeled losses, and missed earnings.
- Contract complexity has outpaced internal capabilities as downside risk expands across Medicare Advantage, Medicaid, and commercial lines.
- Contract modeling and fee schedule math live in manual spreadsheets, which are slow, brittle, and hard to scale.
- Providers rely on payer reporting and lack an independent way to validate shared savings and total cost of care.
- Performance is often evaluated after the year ends, when it is too late to correct course or avoid losses.

- Model shared savings, risk corridors, quality incentives, and attribution rules across all lines of business.
- Quantify expected value, downside exposure, and break‑even points for each scenario in minutes.
- Walk into negotiations with independent, defensible numbers instead of relying on payer assumptions.

You do not need more dashboards. You need clarity into contract economics before, during, and after performance. Syntax shows where you gain or lose dollars so you can act in time. That means you can:
- Monitor performance against contract‑specific benchmarks and catch downside risk mid‑year, not after reconciliation.
- Independently validate shared savings and total cost of care with audit‑ready methods.
- Identify contracts that are accretive, risky, or structurally misaligned and adjust your value‑based care portfolio strategy.
Most organizations can see performance. Very few can translate it into financial truth. Syntax fills the missing layer of contract intelligence and actuarial modeling.
Before you commit capital, understand the game. Syntax uses actuarial modeling to expose hidden risk, validate baselines, and size multi‑year scenarios so you negotiate from strength, not uncertainty.
- Replace manual CPT and fee schedule spreadsheets with one consistent modeling environment.
- Test what‑if scenarios for attribution, exclusions, carve‑outs, and volatility.
- Prepare board‑ready projections of upside, downside, and reserves before you sign.
Many teams can see performance. Very few can translate it into financial truth. Syntax links performance to contract logic so you always know how you track against targets and risk.
- Tie cost, utilization, and quality metrics directly to each contract’s terms and benchmarks.
- Forecast end‑of‑year savings, losses, and earnings potential with actuarial‑grade accuracy.
- Surface early warning signals where contract dynamics put you at risk, not just where clinical metrics slip.
Traditional programs wait for year‑end reconciliation. Syntax supports continuous monitoring and independent validation so you manage performance in real time instead of in hindsight.
- Keep version‑controlled, audit‑ready contract logic and calculations in one place.
- Support payer reconciliation and disputes with transparent and defensible methods.
- Inform stop‑loss strategy, reserve planning, and future contract priorities using real financial signals.
MCR Health
Mitigated Over $1.5M in Downside Risk
By mid‑2024, MCR Health faced more than $1.5 million in downside risk across several unclear value‑based contracts. Syntax helped them model multiple scenarios, clarify contract terms, and identify arrangements that improved projected earnings while reducing downside exposure.
PanCare
Unlocked Over $1 Million in VBC Earnings Potential
PanCare, a community health center active in three value‑based contracts, lacked clear visibility into how performance translated into dollars. Using Syntax, they validated payer assumptions, uncovered areas where they were outperforming expectations, and identified more than $1 million in additional earnings potential.
Syntax adds contract intelligence and actuarial modeling alongside Lightbeam’s population health, care management, and performance solutions to create one connected operating system for value‑based care. Design better contracts, execute programs with the same trusted data, and see financial and clinical results in a single view. Our actuarial and contracting experts support your team at each step so you build a repeatable, in‑house operating model for value‑based care.
- Use one platform to design contracts, manage risk, and measure outcomes across Medicare, Medicaid, and commercial programs.
- Give finance, contracting, clinical, and operations teams a shared source of truth instead of separate tools and spreadsheets.
- Turn insights into action faster by tying contract economics to the population health, care management, and performance workflows that power your value‑based care programs, including those supported by Lightbeam.
Run value‑based care on one platform that brings contract intelligence, population health, and performance together, so your strategy stays clear, actionable, and financially strong.